Despite delivering, with few exceptions, the highest life expectancy outside the OECD, the GCC healthcare industry is still in its infancy.
It has fewer than 60,000 hospital beds and just over two for each 1,000 people living in the region.
This is less than half the ratio in Europe and North America. The GCC devotes little more than 2 per cent of its GDP to healthcare. It’s above 15 per cent in the US and about 10 per cent in Western Europe. But this is about to change.
GCC governments are enjoying an oil windfall and Gulf household incomes have doubled in a decade. They are both increasing spending on health. Demand for healthcare is also being driven higher by the diseases of affluence now afflicting the people of the region.
And not long from now, some of the Gulf baby boomers born during the region’s first oil price boom will be pensioners.
According to a 2005 report by McKinsey & Company, healthcare is the region’s fastest-growing market. It will increase to nearly $30,000 million in 2015 and close to $60,000 million in 2025. A report last year by SRI for the Saudi Arabian General Investment Authority (Sagia) forecast Saudi Arabia will need almost 40 per cent more beds and doctors within a decade.
GCC government and business are responding with the largest hospital building programme in Middle East history. In Dubai, which has the most ambitious plans in the GCC, the number of beds will rise by 70 per cent from just under 3,000 now to more than 4,400 in 2010.
More of them will be private. Two-thirds of the additional beds in Dubai by 2010 will be in non-government establishments. By that date, for-profit hospitals will account for 45 per cent of the total. The public sector too is stepping up its capital investment.
But it’s not all good news for the GCC healthcare industry. There is insufficient demographic data to support coherent long-term healthcare planning and worry that the GCC may be overinvesting in hospital capacity.
This is prompting forecasts of growing competition for patients between public and private hospitals. Governments worry private hospitals will skim off high-value patients and leave the state to deal with the poor and long-term care. Everyone fears fragmentation will undermine large, general hospitals that benefit from economies of scale. The end result could be inefficiency, worse services and higher health costs.
The most striking example of the fragmentation of the GCC health system is in the UAE. The federal government is encouraging private investment. Abu Dhabi and Dubai have contributed to the disintegration by establishing their own health departments to run primary, secondary and tertiary networks. In Dubai, Dubai Healthcare City and Dubiotech, a free zone hosting research clinics, create additional complications for national health service planners.
Health policy thinkers are also troubled by the increasingly uneven distribution of high-quality healthcare. The best hospitals are in the GCC’s main cities, but the greatest needs are usually in the hinterlands where private investors won’t go. Abu Dhabi’s desire to create the world’s finest health system could lead to further migration from the poorer emirates. This pattern is being repeated across Arabia.
And then there is the capacity question. The GCC’s reliance on foreign health workers is bound to increase, at least in the short-term. In an attempt to fill the labour gap, Qatar has established the Weill Cornell Medical Centre in Education City as part of the Qatar Foundation programme. It is the world’s first foreign branch of a major US teaching hospital, but its output is limited. Its first batch of doctors graduates in 2008, but there are only 16.
The uncertainties weighing on the region’s healthcare are prompting calls for GCC hospital programme co-ordination to avoid unnecessary duplication and fill health service gaps. A regional approach would also help set standards, create IT links and develop the pharmacy chains modern healthcare requires.
But there is already GCC consensus that governments cannot cover all healthcare costs. The response, however, has varied. Abu Dhabi is the first in the region to launch a comprehensive health insurance system and adopt private finance methods in its hospitals. Others, less convinced by the model, are studying the results.
In health, there are no easy answers. The GCC will need more, and soon, as a healthcare revolution sweeps Arabia.
You might also like...

Contractors win Oman Etihad Rail packages
23 April 2024
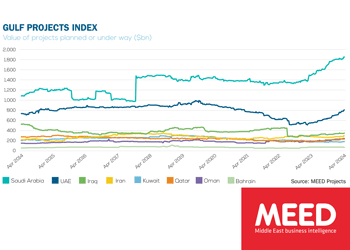
Saudi market returns to growth
23 April 2024
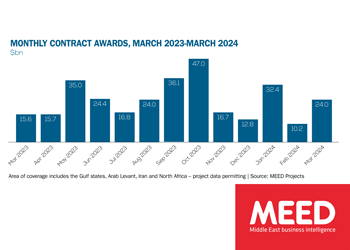
Middle East contract awards: March 2024
23 April 2024

Swiss developer appoints Helvetia residences contractor
23 April 2024
A MEED Subscription...
Subscribe or upgrade your current MEED.com package to support your strategic planning with the MENA region’s best source of business information. Proceed to our online shop below to find out more about the features in each package.